I want to share two numbers with you. Just sit with them for a moment before we go any further.
The first: the UK care sector is facing one of the most serious staffing shortages it has ever seen. Vacancies remain stubbornly high, agency costs are eating into already tight margins, and good people are leaving faster than they can be replaced.
The second: research consistently shows that unemployment among neurodivergent people runs as high as 80%. And when neurodivergent individuals do find work, they’re often in roles that don’t come close to making use of what they’re actually capable of.
Two very different problems.
But here’s the thing.
They are not separate problems at all. They are two sides of the same coin, and the care sector sits in the middle of both, with most leaders never having connected the dots.
This blog is about why that matters, and what you can do about it.
Two Numbers Every Care Leader Should Sit With in the Staffing Crisis
Let’s put those figures into context.
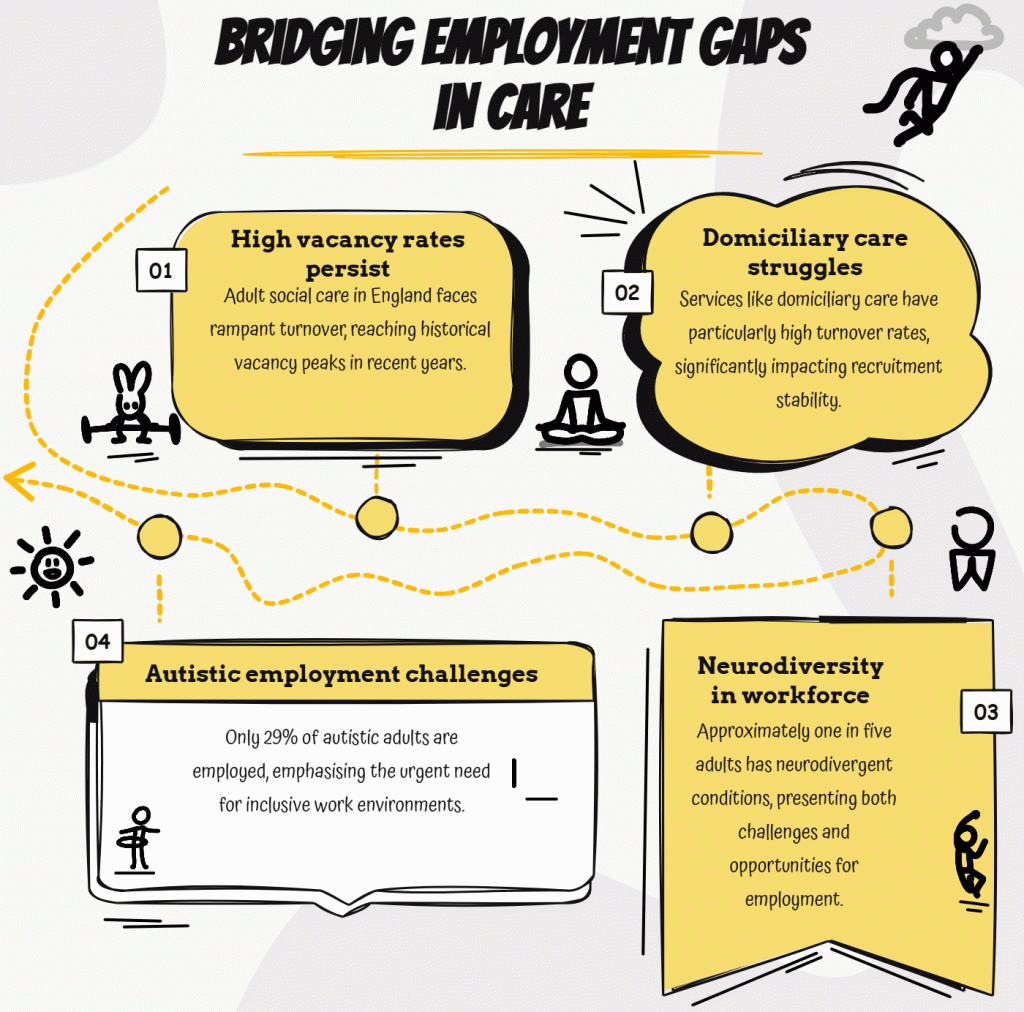
Skills for Care data show that vacancies in adult social care in England peaked at around 165,000 in 2021/22, the highest ever recorded, and have remained consistently above 130,000 since then.
Turnover across the sector averages 28-30%, with some services, particularly domiciliary care, exceeding 35%. Leaders are spending significant money and time on recruitment, only to find themselves back in the same position six months later.
At the same time, neurodivergent people, those with autism, ADHD, dyslexia, dyspraxia, and related conditions, make up around one in five of the working-age population.
Yet a significant proportion are either out of work entirely or working in roles far below their capability. For autistic adults specifically, the ONS puts the employment rate at just 29%.
For others, underemployment, job mismatch, and being stuck in roles that don’t reflect their actual abilities are consistently reported patterns in the research.
That is not a coincidence you can afford to ignore.
Why the Care Sector Hasn’t Connected These Dots Yet
To be clear, this isn’t about blame. Most care leaders I speak to are working incredibly hard just to keep services stable.
Neurodiversity as a workforce strategy simply hasn’t been part of the conversation in this sector the way it has in tech, finance, or professional services.
There are also some honest concerns that come up when I raise this topic with care leaders.
“What if I get it wrong?” “Is it safe to have neurodiverse employees in a care environment?” “Won’t it create more pressure on managers who are already stretched?“
These are reasonable questions. But the assumptions behind them don’t hold up when you look at the evidence, and the cost of not asking them is now significant.
The risk isn’t in recruiting neurodiverse people. The risk lies in continuing to recruit from an ever-shrinking pool while a solution sits right in front of you.
What Neurodiverse Employees Actually Bring to Care Work
Here’s what tends to surprise care leaders when we talk about this properly.
Many of the qualities that make someone genuinely excellent in a care role are exactly the qualities that neurodiverse people often bring in abundance.
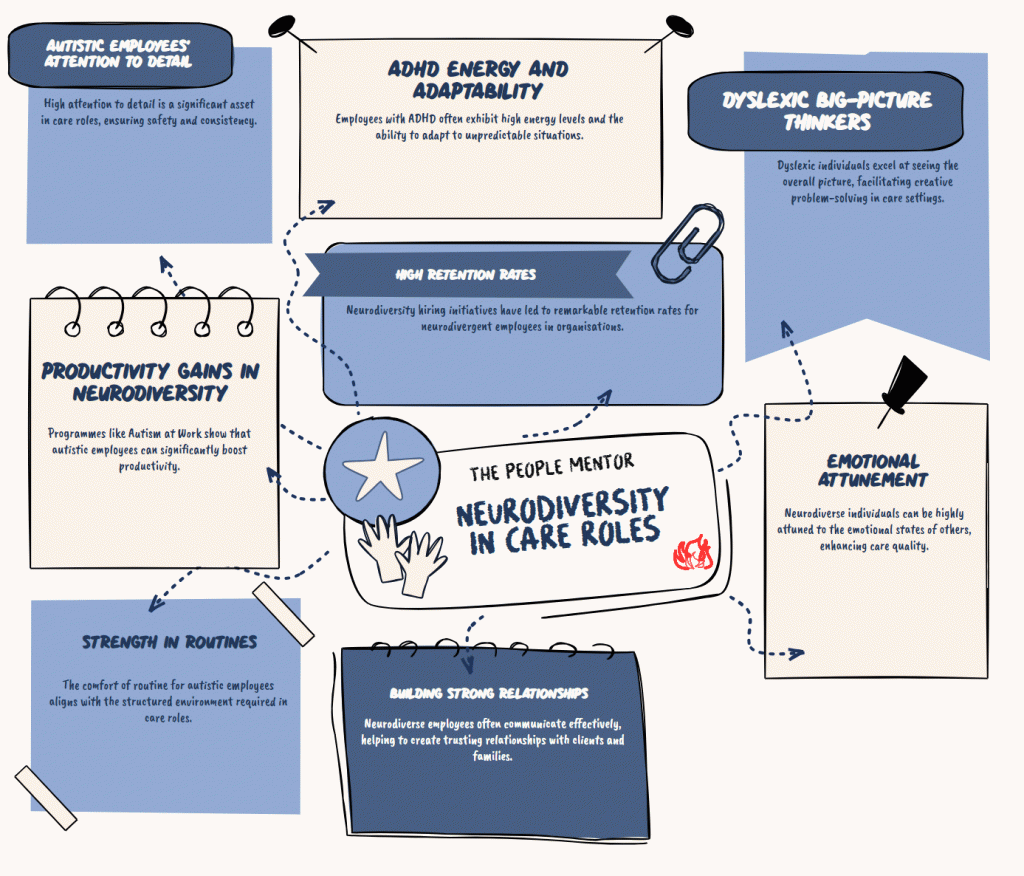
Autistic employees, for example, frequently demonstrate exceptional attention to detail, a deep commitment to consistency and routine, and a high degree of honesty. In a care environment where safe practice depends on exactly these things, those are not minor advantages. They are operationally significant.
People with ADHD often bring real energy, warmth, and the ability to respond well in unpredictable situations. They can be highly attuned to other people’s emotional states. In direct care work, that matters enormously.
Dyslexic thinkers tend to excel at big-picture understanding and creative problem-solving. They often build strong relationships and communicate in ways that residents, clients, and families find reassuring and human.
JPMorgan’s Autism at Work programme found that autistic employees in certain specialist roles delivered nearly 50% higher productivity within just six months compared to neurotypical peers.
SAP launched its own neurodiversity hiring programme back in 2013 and reports retention rates close to 90% for neurodivergent hires, far above anything the sector typically sees. They didn’t do this out of goodwill. They did it because the commercial case was undeniable.
The talent is there. It always has been. What’s been missing is the management approach to bring it out.
Why Neurodiverse Care Workers Are Leaving Before You Get the Benefit
This is the part that keeps me awake a little.
Even when neurodiverse people do find their way into care work, many leave quickly or never reach their potential, not because the role is wrong for them, but because the environment doesn’t account for how they work best.
It often starts before they even arrive. Most care job adverts are dense, full of vague requirements such as excellent communication skills and the ability to work in a fast-paced environment. These phrases, while well-intentioned, read as barriers to many neurodiverse candidates who aren’t sure whether they fit, and decide not to apply.
The interview process then compounds the problem. A panel interview with multiple people firing questions in a busy room, with no advance information about what to expect, is genuinely difficult for many autistic or anxious candidates.
You may be screening out the very person who would be your most reliable and dedicated team member.
And then, once someone is in post and struggling without the right support, the result is almost always masking. They spend their working day suppressing how their brain naturally works, trying to fit a mould that wasn’t designed for them.
That is exhausting in any workplace. In care, where the emotional and sensory demands are already high, it leads to burnout faster than you would believe.
You end up with exactly the turnover problem you were trying to solve.
The cost of small, thoughtful adjustments is minimal. The cost of replacing a member of staff in adult social care, when you factor in recruitment, agency cover, and training, is estimated at several thousand pounds per person. The maths is not complicated.
What You Can Do Differently, Starting This Week
None of what follows requires a formal programme, a policy overhaul, or a budget. It requires attention and a willingness to do things slightly differently.
Write job ads that don’t put people off before they apply
Read your current adverts as if you were someone who thinks literally and takes language at face value. Remove vague phrases. Be specific about what the role actually involves.
State clearly what the interview process will entail and who will be present. This simple change improves applications from neurodiverse candidates and, frankly, from many neurotypical candidates too.
Change how you interview
Consider sharing questions in advance. Allow candidates to bring notes. Offer a brief tour of the environment before the formal interview starts so that unfamiliar sensory elements don’t derail the conversation.
You don’t need to label this as a neurodiversity adjustment. You can simply call it a better interview process, because that’s what it is.
Make the adjustments that actually matter in a care environment
In a shift-based setting, clear written handover notes matter. Consistent routines matter. Not being surprised by last-minute rota changes matters. Most of these are good practices for everyone on the team, not special treatment for a few.
If someone tells you they find the noise of a busy communal area difficult, consider whether there are parts of the role that can flex around that.
Reasonable adjustments under the Equality Act are not about bending the rules. They’re about removing barriers that have nothing to do with whether someone can do the job well.
Create the conditions that keep people
Regular one-to-ones where your team member can ask questions and flag what isn’t working. Clear expectations written down, not just said once at induction. Feedback that is specific and honest rather than vague and softened.
These are things I talk about constantly in my work with care leaders because they improve performance across the whole team. For neurodiverse employees, it can be the difference between thriving and quietly disappearing.
This Isn’t About Running a Special Programme
I want to be direct about something, because I think it matters.
Supporting neurodiverse employees in your care service is not a diversity initiative. It’s not a box to tick for your next inspection, although a genuinely inclusive workplace will absolutely be noticed by CQC under the Well-Led framework.
It is simply good leadership.
When you recruit more thoughtfully, support people more effectively, and create an environment where everyone can do their best work, you get better retention, stronger consistency, and a more stable service. Those outcomes are exactly what every care leader I have ever worked with is looking for.
The neurodivergent talent pool is large, largely overlooked by your sector, and full of people who, given the right conditions, bring real commitment and real capability to care work.
The staffing crisis is real. The solution is at least partially sitting right in front of you.
The question is whether you’re ready to look at it differently.
If you want to understand more about how to communicate effectively with neurodiverse team members, have a read of What Every Manager Needs to Know About Neurodiversity and Untapped Talent and Is Your Workplace Culture Actually Welcoming Neurodiverse People? where I go into more detail on what this looks like in practice.
And if you’d like to talk through what this could mean for your service specifically, you’re very welcome to book a call. I’d love to help you think it through.

